Ear numbness following rhytidectomy procedures represents one of the most frequently encountered complications in facial plastic surgery, affecting approximately 6-7% of patients undergoing facelift operations. This temporary alteration in sensation occurs due to the intricate relationship between surgical dissection planes and the complex network of sensory nerves that innervate the auricular region. Understanding the anatomical basis, clinical implications, and recovery patterns of post-facelift auricular numbness is essential for both surgeons and patients navigating the postoperative period. The phenomenon encompasses a spectrum of sensory disturbances, from complete anaesthesia to paraesthesia, with varying degrees of functional impact on patient comfort and satisfaction.
Anatomical basis of ear numbness following rhytidectomy procedures
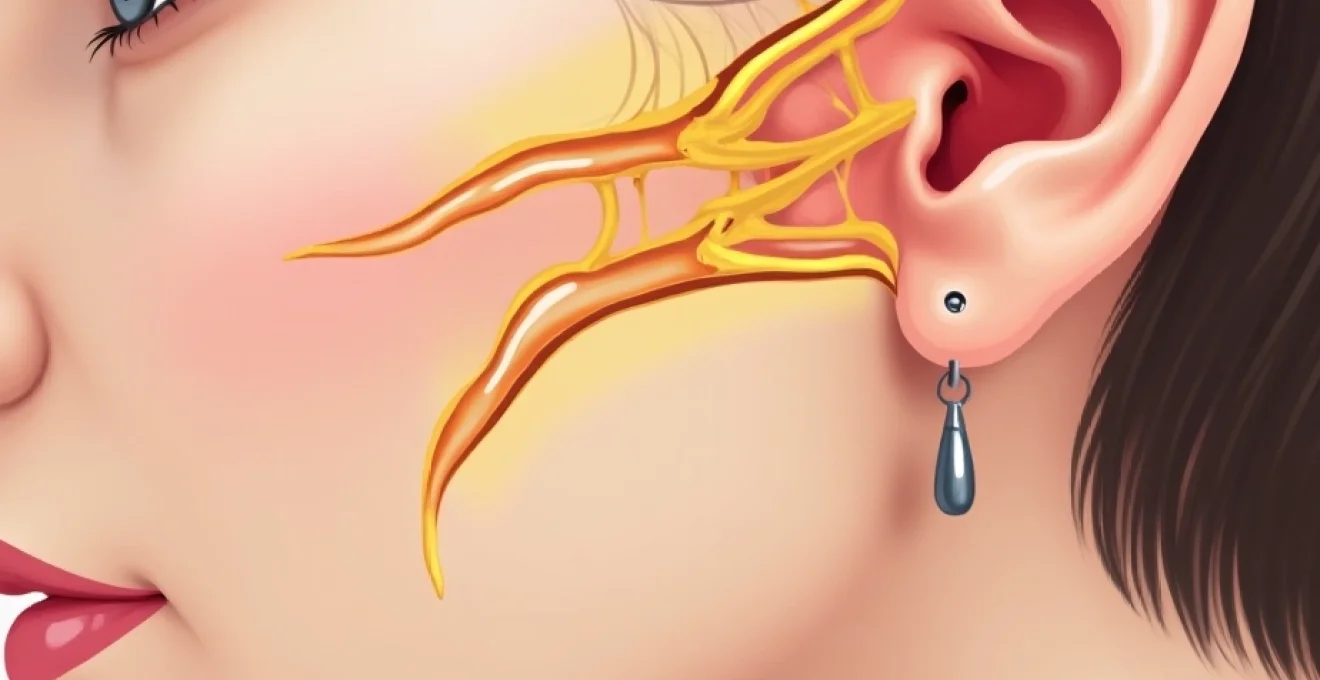
The development of auricular numbness after facelift surgery stems from the complex anatomical relationship between surgical dissection planes and the peripheral nervous system supplying the ear and surrounding tissues. The sensory innervation of the external ear involves multiple nerve branches originating from both the cervical plexus and cranial nerves, creating a delicate network that can be vulnerable during facial rejuvenation procedures. Understanding this anatomical foundation provides crucial insight into why ear numbness occurs and helps predict recovery patterns for affected patients.
Greater auricular nerve distribution and surgical vulnerability
The greater auricular nerve, originating from the cervical plexus (C2-C3), represents the primary sensory supply to the external ear and constitutes the most commonly injured nerve during facelift procedures. This nerve travels superficially along the anterior border of the sternocleidomastoid muscle before ascending to innervate the earlobe and lower portion of the external ear. During rhytidectomy, the nerve’s superficial course places it at significant risk during skin undermining and SMAS manipulation, particularly when surgical dissection extends into the neck region. The greater auricular nerve’s anatomical variability between patients further complicates surgical planning, as some individuals may have branches that extend more anteriorly than typical anatomical descriptions suggest.
Superficial musculoaponeurotic system (SMAS) dissection impact on sensory innervation
SMAS layer manipulation during facelift surgery can significantly affect sensory nerve function through both direct trauma and secondary compression mechanisms. The SMAS contains embedded nerve fibres and serves as a protective layer for deeper sensory branches, meaning that aggressive SMAS elevation or plication can result in neuropraxia or more severe nerve injury. Modern facelift techniques that involve extensive SMAS mobilisation may inadvertently stretch or compress sensory nerve branches, leading to temporary or permanent alterations in auricular sensation. The relationship between SMAS thickness and nerve protection varies among individuals, with patients having thinner SMAS layers potentially experiencing higher rates of sensory complications.
Cervical plexus branch involvement in Post-Facelift paraesthesia
Beyond the greater auricular nerve, additional branches of the cervical plexus contribute to auricular sensation and may be affected during facelift surgery. The lesser occipital nerve and transverse cervical nerve branches can influence sensation around the posterior and inferior aspects of the external ear, respectively. These nerves travel in close proximity to common facelift incision sites, making them susceptible to injury during surgical approach and closure. The interconnected nature of cervical plexus branches means that injury to one component can affect the overall sensory perception of the entire auricular region, contributing to the complex pattern of numbness experienced by some patients.
Temporal branch facial nerve proximity during lateral SMASectomy
During lateral SMASectomy procedures, the temporal branch of the facial nerve may be encountered in the dissection plane, though this motor nerve primarily affects muscle function rather than sensation. However, the close anatomical relationship between motor and sensory nerve fibres in this region means that surgical trauma affecting the temporal branch can indirectly influence sensory perception through inflammatory responses and tissue oedema. The temporal region’s complex innervation pattern includes sensory contributions from the auriculotemporal nerve, which can be affected by extensive temporal dissection during comprehensive facelift procedures.
Intraoperative factors contributing to Post-Rhytidectomy auricular hypoaesthesia
Multiple technical and procedural factors during facelift surgery can contribute to the development of auricular numbness, with the extent and duration of sensory loss often correlating with the degree of surgical trauma sustained by peripheral nerves. Understanding these contributing factors enables surgeons to modify their technique to minimise nerve injury while still achieving optimal aesthetic outcomes. The interplay between surgical approach, tissue handling, and individual patient anatomy creates a complex risk profile that requires careful consideration during operative planning.
Extended SMAS techniques and increased neuropraxia risk
Extended SMAS lifting techniques, while providing superior aesthetic results in terms of longevity and natural appearance, inherently carry increased risk of sensory nerve injury due to more extensive tissue dissection. These advanced techniques require elevation of the SMAS layer over a broader area, increasing the likelihood of encountering and potentially traumatising sensory nerve branches. The deep plane facelift, composite facelift, and extended lateral SMASectomy all involve dissection in anatomical planes that bring surgical instruments into close proximity with key sensory nerves. The trade-off between aesthetic enhancement and sensory preservation requires careful surgical judgement and precise anatomical knowledge.
Electrocautery-induced thermal injury to sensory branches
The use of electrocautery devices during facelift surgery, while essential for haemostasis and tissue dissection, can cause thermal injury to nearby sensory nerves even when direct contact is avoided. The conduction of electrical current through tissues can damage nerve fibres through heat generation, leading to neuropraxia or axonotmesis depending on the severity of thermal injury. Bipolar electrocautery, while generally safer than monopolar devices, still carries risk of collateral nerve damage when used in close proximity to sensory branches. The cumulative effect of multiple brief electrocautery applications can result in significant thermal injury to delicate nerve structures, particularly in the thin tissues around the external ear.
Excessive skin undermining in the preauricular region
Aggressive skin undermining in the preauricular region can stretch sensory nerve branches beyond their elastic limit, resulting in mechanical nerve injury and subsequent numbness. The balance between achieving adequate skin mobility for tension-free closure and preserving nerve integrity requires precise surgical technique and anatomical awareness. Blunt dissection techniques, while generally safer for nerve preservation than sharp dissection, can still cause significant mechanical trauma if applied with excessive force or in inappropriate tissue planes. The preauricular skin’s adherence to underlying structures varies among patients, influencing the degree of undermining required and the associated risk of nerve injury.
Deep plane facelift complications affecting auricular sensation
Deep plane facelift techniques, which involve dissection beneath the SMAS layer, place sensory nerves at particular risk due to the proximity of the dissection plane to nerve pathways. The subSMAS space contains numerous small sensory branches that can be inadvertently divided or stretched during deep plane elevation. The technical complexity of deep plane dissection requires exceptional surgical skill to navigate around vital structures while maintaining the tissue planes necessary for optimal aesthetic results. Complications in this deeper anatomical layer often result in more persistent sensory deficits compared to superficial plane injuries.
Postoperative oedema and compression neuropathy development
Postoperative tissue swelling can contribute to sensory nerve dysfunction through compression mechanisms, even when direct surgical trauma has been minimal. The confined anatomical spaces around the external ear provide limited room for tissue expansion, meaning that even modest amounts of oedema can result in significant pressure on sensory nerve branches. This compression neuropathy can persist for weeks or months following surgery, contributing to prolonged sensory deficits. The relationship between postoperative haematoma formation and nerve compression represents a particular concern, as expanding haematomas can cause both mechanical compression and ischaemic injury to affected nerves.
The incidence of greater auricular nerve injury during facelift surgery ranges from 6% to 7% in published studies, with most patients experiencing gradual recovery of sensation over 6-12 months postoperatively.
Clinical presentation and differential diagnosis of auricular numbness
The clinical presentation of auricular numbness following facelift surgery encompasses a spectrum of sensory disturbances that can vary significantly between patients in terms of severity, distribution, and associated symptoms. Patients typically report decreased sensation ranging from mild hypoaesthesia to complete anaesthesia in the affected auricular region. The numbness commonly involves the earlobe, external auditory canal, and surrounding preauricular skin, though the exact pattern depends on which specific nerve branches have been affected during surgery. Some patients may experience paraesthesia, described as tingling, burning, or “pins and needles” sensations, which often indicate recovering nerve function.
The temporal evolution of symptoms provides important diagnostic information, with immediate postoperative numbness typically indicating direct nerve trauma, while delayed onset may suggest compression from developing oedema or haematoma. Patients frequently report that the numbness is most noticeable when touching the affected area or during activities such as wearing earrings or using telephone headsets. The subjective nature of sensory complaints requires careful clinical assessment to distinguish between normal postoperative changes and pathological nerve injury requiring intervention.
Differential diagnosis must consider other potential causes of auricular numbness, including infection , haematoma formation, excessive tension on closure, or pre-existing neurological conditions. The unilateral nature of symptoms following facelift surgery helps distinguish nerve injury from systemic neurological disorders, while the temporal relationship to surgery supports a causal connection. Clinical examination should assess both light touch and pinprick sensation, comparing affected areas to the contralateral normal side to quantify the degree of sensory loss objectively.
Recovery timeline and neuroregeneration patterns after facelift surgery
Understanding the natural history of nerve recovery following facelift surgery provides essential information for patient counselling and clinical management decisions. The regeneration process follows predictable biological patterns, though individual variation in healing responses can result in significant differences in recovery timelines between patients. Most sensory recovery occurs through spontaneous nerve regeneration mechanisms, with the degree and speed of recovery depending on the severity of initial nerve injury and individual patient factors.
Wallerian degeneration process in damaged auricular nerves
When sensory nerves sustain significant trauma during facelift surgery, they undergo a process called Wallerian degeneration, where the axon distal to the injury site degenerates and is cleared away by macrophages. This process typically begins within 24-48 hours of injury and can take several weeks to complete, during which time the affected nerve remains non-functional. The severity of initial trauma determines whether the nerve injury represents neuropraxia (temporary conduction block), axonotmesis (axon damage with intact neural tube), or neurotmesis (complete nerve division). Understanding this degenerative process helps explain why immediate nerve repair attempts are generally unsuccessful and why patience is required during the recovery period.
Spontaneous reinnervation mechanisms and expected timeframes
Following Wallerian degeneration, spontaneous nerve regeneration occurs through axonal sprouting from the proximal nerve stump, with new axons growing at approximately 1mm per day towards their target receptors. This regeneration process can take several months to complete, depending on the distance between the injury site and target organs. Clinical evidence of recovery typically begins 2-3 months after surgery, with progressive improvement continuing for up to 12-18 months in some cases. Early signs of recovery include the return of paraesthesia sensations, followed by gradual restoration of normal touch and temperature perception. The quality of recovered sensation may differ from preoperative baseline, with some patients experiencing permanent alterations in sensory perception despite functional recovery.
Factors influencing sensory recovery in Post-Rhytidectomy patients
Multiple factors influence the likelihood and extent of sensory recovery following facelift-associated nerve injury. Patient age represents a significant variable, with younger individuals generally demonstrating superior regenerative capacity compared to older patients. The mechanism and severity of initial nerve injury also critically affect recovery potential, with crush injuries typically healing better than sharp divisions or thermal damage. Systemic factors such as diabetes, smoking history, and nutritional status can impair nerve regeneration through effects on blood supply and cellular metabolism. The development of postoperative complications, including infection or prolonged oedema, can further compromise recovery by creating an unfavourable environment for nerve regeneration.
Management strategies for persistent auricular hypoaesthesia
The management of persistent auricular numbness following facelift surgery requires a multifaceted approach that addresses both the underlying pathophysiology and the patient’s functional concerns. Initial management focuses on supportive care and monitoring for spontaneous recovery, while more aggressive interventions may be considered for cases with prolonged or severe sensory deficits. The timing of intervention is crucial, as premature surgical exploration may interfere with natural healing processes, while delayed treatment may miss opportunities for optimal nerve repair.
Conservative management strategies include patient education about expected recovery timelines, protective measures to prevent injury to anaesthetic skin, and symptomatic treatment for uncomfortable paraesthesia. Topical anaesthetic preparations can provide temporary relief for patients experiencing painful tingling sensations during nerve regeneration. Physical therapy modalities, including gentle massage and sensory re-education exercises, may help optimise functional recovery once regeneration begins. The use of oral medications such as gabapentin or pregabalin can be considered for patients with significant neuropathic pain, though these agents are typically reserved for severe cases due to potential side effects.
For cases of persistent complete anaesthesia beyond 12-18 months, surgical exploration and nerve repair procedures may be considered. Direct nerve anastomosis can be attempted if adequate nerve length is available, while nerve grafting techniques may be necessary for cases involving significant nerve loss. The success of delayed nerve repair procedures is generally limited compared to immediate repair, highlighting the importance of initial surgical technique in preventing nerve injury. Alternative approaches include nerve transfer procedures using nearby functioning sensory branches to restore sensation to the affected area.
Approximately 80-90% of patients with post-facelift auricular numbness experience significant recovery within 6-12 months, with complete resolution occurring in about 70% of cases by 18 months postoperatively.
Prevention protocols and surgical modifications to minimise nerve injury
The most effective approach to managing auricular numbness involves prevention through careful surgical technique and anatomical awareness during facelift procedures. Modern understanding of facial nerve anatomy has led to the development of specific protocols designed to minimise the risk of sensory nerve injury while maintaining the aesthetic benefits of comprehensive facial rejuvenation. These prevention strategies encompass preoperative planning, intraoperative technique modifications, and postoperative care protocols that collectively reduce the incidence and severity of sensory complications.
Preoperative imaging and anatomical mapping can help identify patients with unusual nerve anatomy or previous surgical alterations that may increase the risk of nerve injury. The use of nerve monitoring devices during surgery provides real-time feedback about nerve proximity and can alert surgeons to potential injury before permanent damage occurs. Surgical loupes or microscopic magnification enable precise dissection and improved visualisation of tissue planes, reducing the likelihood of inadvertent nerve trauma. The adoption of incremental advancement techniques, where tissue is mobilised gradually rather than through aggressive single-stage elevation, can reduce mechanical stress on nerve structures.
Modification of electrocautery usage represents another important prevention strategy, with many surgeons advocating for reduced power settings and increased reliance on mechanical haemostasis in areas of high nerve density. The use of bipolar electrocautery devices minimises current spread and reduces the risk of thermal injury to nearby structures. Some surgeons employ “nerve-sparing” techniques that specifically identify and preserve major sensory branches during dissection, though these approaches may require longer operative times and increased technical expertise. The development of endoscopic facelift techniques offers potential advantages in nerve preservation through improved visualisation and reduced tissue trauma, though long-term comparative data regarding sensory outcomes remain limited.
Postoperative protocols aimed at preventing complications that could exacerbate nerve injury include careful monitoring for haematoma formation, aggressive management of postoperative oedema, and early recognition of signs suggesting nerve compression. The use of corticosteroids in the immediate postoperative period remains controversial, with some evidence suggesting potential benefits for nerve recovery while other studies show no significant improvement in outcomes. Patient education regarding realistic expectations and the natural history of nerve recovery helps reduce anxiety and improves satisfaction with surgical outcomes, even when temporary sensory changes occur. Long-term follow-up protocols ensure that patients with persistent sensory deficits receive appropriate evaluation and management, contributing to improved overall outcomes in facial plastic surgery practice.